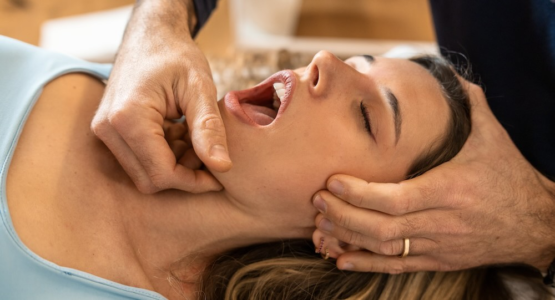
Temporomandibular joint (TMJ) dysfunction affects the jaw joints and surrounding muscles, causing symptoms such as jaw pain, clicking or popping sounds, limited mouth opening, headaches, and facial pain that can significantly impact eating, speaking, and quality of life. TMJ disorders can result from various factors including teeth grinding or clenching (bruxism), jaw trauma, arthritis, stress-related muscle tension, poor posture, or misalignment of the jaw joints. The condition often involves complex interactions between the jaw muscles, cervical spine, and overall posture, making it well-suited for physiotherapy intervention. Physiotherapy for TMJ dysfunction begins with a comprehensive assessment of jaw movement, muscle tension, posture, and cervical spine function to identify contributing factors and develop an individualized treatment plan. Treatment typically includes manual therapy techniques such as gentle joint mobilization and soft tissue massage to reduce muscle tension and improve jaw mobility, specific exercises to strengthen weak jaw muscles and stretch tight structures, postural correction to address neck and shoulder positioning that affects jaw function, and relaxation techniques to manage stress and reduce muscle clenching. Physiotherapists also provide education about jaw-friendly eating habits, proper sleep positioning, stress management strategies, and ergonomic modifications to work environments that may contribute to jaw tension and dysfunction.
Frequently Asked Questions:
1. How does physiotherapy help with TMJ pain, and what techniques are used? Physiotherapy helps TMJ pain through a combination of manual therapy techniques and targeted exercises that address both the jaw joint itself and related structures. Your physiotherapist will use gentle intraoral and extraoral manual techniques to mobilize the temporomandibular joint, reduce muscle tension in the jaw muscles (masseter, temporalis, and pterygoids), and improve joint mechanics. Treatment often includes soft tissue massage to release trigger points in the jaw and neck muscles, gentle stretching exercises to improve mouth opening and jaw mobility, and coordination exercises to retrain proper jaw movement patterns. Additionally, since the cervical spine and posture significantly influence TMJ function, your treatment will likely include neck mobilization, postural correction exercises, and techniques to address any restrictions in the upper cervical region that may be contributing to your jaw dysfunction.
2. Why does my neck and posture affect my TMJ, and how does physiotherapy address this connection? The relationship between your neck, posture, and TMJ is biomechanically interconnected through shared muscle attachments, fascial connections, and neurological pathways. Forward head posture, commonly seen in people who work at computers or look down at phones frequently, places the cervical spine in extension and can alter the resting position of the jaw, leading to increased tension in the jaw muscles. Poor posture also affects the hyoid bone and tongue positioning, which influences jaw function. Your physiotherapist will assess your posture from head to toe, identifying issues like rounded shoulders, forward head posture, or thoracic kyphosis that contribute to TMJ problems. Treatment includes strengthening exercises for the deep neck flexors and upper back muscles, stretching tight chest and neck muscles, ergonomic education for workspace setup, and postural awareness training to help you maintain better alignment throughout the day.
3. What exercises can I do at home to help my TMJ symptoms? Home exercises for TMJ typically focus on gentle mobility, strengthening, and relaxation techniques that you can safely perform independently. Common exercises include gentle jaw opening exercises where you place your tongue on the roof of your mouth and slowly open and close your jaw, lateral jaw movements where you move your jaw side to side in a controlled manner, and resistance exercises using your hand to provide gentle opposition during jaw opening or closing. Relaxation exercises are equally important and may include gentle jaw massage, warm compress application, and stress-reduction techniques like deep breathing or progressive muscle relaxation. Your physiotherapist will also teach you postural exercises like chin tucks to improve neck alignment, upper back strengthening exercises, and stretches for the neck and shoulder muscles. It’s crucial to perform these exercises gently and stop if you experience increased pain, as aggressive stretching can worsen TMJ symptoms.
4. How long does physiotherapy take to improve TMJ dysfunction, and what can I expect during treatment? TMJ dysfunction recovery varies significantly depending on the severity of your condition, underlying causes, and contributing factors, but most patients begin to notice some improvement within 4-6 weeks of consistent treatment. Acute TMJ problems may resolve within 6-8 weeks, while chronic conditions that have been present for months or years may require 12-16 weeks or longer to achieve substantial improvement. During treatment, you can expect initial sessions to focus on pain reduction and gentle mobility restoration, followed by progressive strengthening and postural correction as symptoms improve. Your physiotherapist will likely recommend 1-2 sessions per week initially, with treatment frequency decreasing as you improve and learn to manage symptoms independently. Progress may include reduced pain intensity, increased mouth opening, decreased clicking or popping sounds, improved chewing function, and reduced frequency of headaches. Your physiotherapist will also work with you to identify and modify habits or lifestyle factors that contribute to your TMJ dysfunction, ensuring long-term success and preventing recurrence.