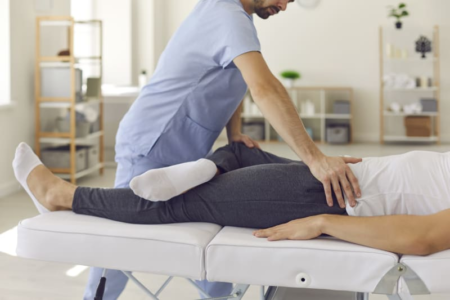
Chronic pain, defined as pain persisting for more than three to six months beyond normal tissue healing time, affects millions of people worldwide and represents a complex condition that involves changes in both the peripheral and central nervous systems. Unlike acute pain that serves as a protective warning signal, chronic pain often persists even after the original injury has healed, becoming a condition in itself that can significantly impact physical function, mental health, and overall quality of life. Physiotherapy offers a comprehensive, evidence-based approach to chronic pain management that goes beyond simply treating symptoms to address the underlying mechanisms that perpetuate pain. Modern physiotherapy for chronic pain incorporates pain neuroscience education to help patients understand how pain works and why it persists, graded exercise therapy to gradually rebuild physical capacity without fear of movement, manual therapy techniques to address tissue restrictions and nervous system sensitivity, and cognitive-behavioral strategies to develop effective coping mechanisms. Treatment focuses on desensitizing the nervous system, improving physical function, reducing fear-avoidance behaviors, and empowering patients with self-management tools including pacing strategies, stress management techniques, and lifestyle modifications. Physiotherapists work collaboratively with patients to set realistic goals, gradually increase activity levels, and develop sustainable exercise programs that not only reduce pain intensity but also improve sleep, mood, and overall well-being.
Frequently Asked Questions:
1. How is treating chronic pain different from treating acute injuries, and why does it take longer? Chronic pain treatment differs fundamentally from acute injury management because chronic pain involves complex changes in your nervous system that go beyond the original tissue damage. While acute pain treatment focuses on healing injured structures, chronic pain physiotherapy addresses how your brain and nervous system process pain signals, which have become hypersensitive over time. The nervous system essentially “learns” to produce pain more easily and intensely, even in response to normal stimuli. Recovery takes longer because you’re not just healing tissues – you’re retraining your nervous system to respond more normally to everyday activities and sensations. This neuroplastic change requires consistent, patient effort over months rather than weeks, with progress often occurring in small increments rather than dramatic improvements, making patience and persistence essential components of successful treatment.
2. Will exercise make my chronic pain worse, and how do I know what activities are safe? This is one of the most common concerns, and it’s understandable given that movement may initially increase your pain. However, research consistently shows that gradually increasing activity and exercise is one of the most effective treatments for chronic pain. Your physiotherapist will use a “graded exposure” approach, starting with very gentle activities well within your tolerance and slowly building up intensity and duration. The key is distinguishing between hurt and harm – some discomfort during activity is normal and doesn’t indicate tissue damage in chronic pain conditions. Your physiotherapist will teach you to recognize your baseline pain levels, understand that temporary increases in pain don’t mean you’re causing injury, and use pacing strategies to gradually expand your activity tolerance while avoiding boom-bust cycles that can perpetuate the pain experience.
3. What is pain neuroscience education, and how does understanding my pain help reduce it? Pain neuroscience education involves learning how your pain system actually works, which can be incredibly empowering and therapeutic in itself. Many people with chronic pain believe their pain means ongoing tissue damage, leading to fear and avoidance that actually worsens the condition. Understanding that chronic pain often reflects a hypersensitive nervous system rather than ongoing injury helps reduce fear and catastrophic thinking about your condition. Your physiotherapist will explain concepts like central sensitization, where your nervous system becomes overly protective and generates pain signals even when there’s no real threat to your tissues. This knowledge helps you understand why activities that were once painful can become tolerable again, why pain levels can fluctuate seemingly randomly, and why a multifaceted approach including movement, stress management, and lifestyle changes is necessary for recovery.
4. How do I maintain progress with chronic pain management, and what happens if I have setbacks? Maintaining progress with chronic pain requires developing a sustainable self-management approach that becomes part of your daily routine. Your physiotherapist will teach you to recognize early warning signs of flare-ups, implement pacing strategies that balance activity with rest, and maintain a regular exercise routine that preserves your gains. Setbacks are a normal part of chronic pain recovery and don’t indicate failure or permanent regression – they’re opportunities to practice your coping strategies and reinforce your understanding of pain management principles. When setbacks occur, your physiotherapist will help you identify potential triggers such as stress, changes in sleep, or overdoing activities, and adjust your management plan accordingly. Long-term success comes from building confidence in your ability to manage symptoms independently, maintaining realistic expectations about the recovery process, and having a toolkit of strategies you can implement when challenges arise.